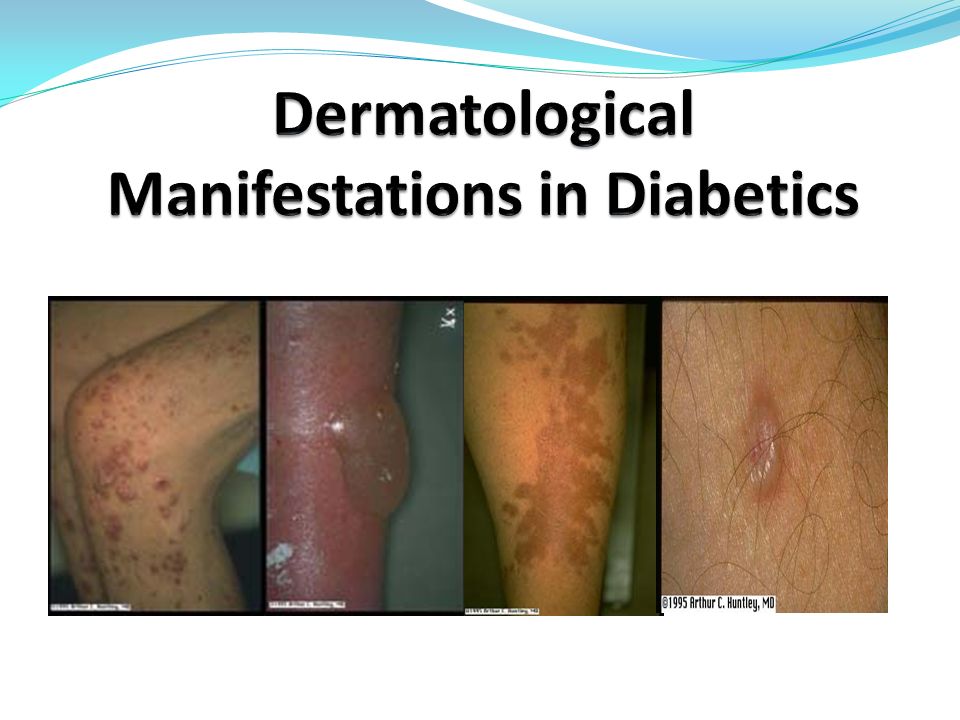
Doctors of various specialties, including endocrinologists, encounter pathological changes in the skin. Skin lesions can be either an accidental find or the main complaint of a patient. Innocent at first glance, skin changes may be the only sign of a serious illness. The skin is the most accessible organ for research and at the same time a source of vital information. Skin lesions can clarify the diagnosis in many internal diseases, including diabetes mellitus (diabetes mellitus).
Skin changes with Diabetes mellitus is quite common. Severe metabolic abnormalities underlying the pathogenesis of diabetes mellitus lead to changes in almost all organs and canes, including the skin.
Some diabetes-associated skin symptoms are a direct result of metabolic changes, such as hyperglycemia and hyperlipidemia. Progressive damage to the vascular, nervous, or immune systems also contributes significantly to the development of skin manifestations. The mechanisms of other diabetes-associated dermatological lesions remain unknown.
Promote skin changes can also hyperinsulinemia, as is the case in the early stages of insulin-resistant type 2 diabetes.
Significantly worsen during cutaneous complications of diabetes Makr o- and microangiopathy. In patients with diabetes, there is an increased “leakage” or permeability of the vascular wall, a decrease in vascular reactivity for sympathetic innervation and hypoxemic stress. In combination with arteriosclerosis of large vessels, these microvascular disorders contribute to the formation of diabetic ulcers. In addition, diabetes develops a loss of skin innervation sensitivity, which predisposes to infections and injuries. As a rule, diabetic skin lesions have a long and persistent course with frequent exacerbations and are difficult to treat.
There are several classifications of skin lesions with Diabetes mellitus, they are based on clinical characteristics and some aspects of the pathogenesis of skin changes. It’s like skin pathology with Diabetes mellitus is divided into five main groups:
1) dermatosis associated with diabetes mellitus;
2) skin pathology associated with diabetes mellitus and insulin resistance;
3) skin pathology associated with angiopathy;
4) idiopathic rash;
5) bacterial and fungal infections.
In the classification described by Andrea A. Kalus , Andy J. C hien , John E. Olerud (2012) , the following groups of diabetes-associated skin lesions are distinguished:
1) cutaneous manifestations of diabetes associated with metabolic, vascular, neurological, or immune disorders (diabetic scleredema, acanthosis nigricans, diabetic thickening of skin, limitation of joint mobility and sklerodermopodobny syndrome, eruptive xanthoma, skin infections (bacterial, fungal), diabetic ulcers);
2) Diseases associated with diabetes mellitus with unclear pathogenesis (lipoid necrobiosis, annular granuloma, diabetic bladder, diabetic dermopathy ).
These classifications practically do not differ and only complement each other.
By dermatoses associated with diabetes include diabetic scleredum. Scleredema is more common with long-term diabetes mellitus in combination with obesity and manifests itself as diffuse, symmetric, indurative skin changes, mainly in the neck and upper third of the back like an orange peel. According to different authors, the frequency of its occurrence in patients with diabetes mellitus is 2.5-14% .
It was expected that the pathogenesis of diabetic scleredema is unregulated production of extracellular matrix molecules by fibroblasts, which leads to thickening of the collagen bundles and increased deposition w glycosaminoglycans (GAGs). Patients with a diabetic scleredema may experience a reduction in pain and light sensitivity in the area of the affected skin areas, as well as complain of difficulties in movements of the upper limbs and neck. In extreme cases, the disease can lead to complete loss of mobility of the joints, however, the presence of scleradema is not associated with retinopathy , nephropathy, neuropathy, or damage to large vessels.
The link with insulin resistance and obesity can be traced with black acantosis ( acantosis nigricans ), which is manifested by areas of skin hyperpigmentation with papillomatous growths in the neck and large folds . Insulin plays a central role in the development of acanthosis. In women suffering from acanthosis , it is possible to detect the loss of functional mutations of the insulin receptor or the receptor of anti-insulin antibodies (with type A and type B indrom ). It is believed that excessive stimulation of growth factor in the skin causes aberrant proliferation of keratinocytes and fibroblasts, as a result of which the clinical manifestations of black acanthosis develop . In conditions of hyperinsulinemia and insulin resistance, acanthosis may develop due to excessive insulin binding to IGF receptors – 1 to eratinotsitah and fibroblasts. Evidence in favor of the role of various growth factors in the pathogenesis of black acanthosis continues to accumulate.
Undiagnosed Diabetes mellitus and hypertriglyceridemia can provoke eruptive appearance on the skin. xantom [46, 8]. They are reddish-yellow papules with a size of 1-4 mm., Located on the buttocks and extensor surfaces of the extremities. Pathological elements appear in the form of grains and may eventually merge to form plaques. Initially, triglycerides predominate in the skin elements, but since they mobilize more easily than cholesterol, with their disintegration, more and more cholesterol accumulates in the skin.
Insulin is an important regulator of LDL activity. The degree of enzyme deficiency and subsequent purification of serum triglycerides is proportional to the indicators of insulin deficiency and hyperglycemia. The clearance of plasma lipoproteins depends on adequate insulin levels. In uncontrolled diabetes, such an inability to metabolize and release triglyceride-rich chylomicrons and very low density lipoproteins can lead to an increase in plasma triglycerides to several thousand. Uncontrolled diabetes is a common cause of massive hypertriglyceridemia.
Patients with diabetes are prone to the development of skin infectious diseases, especially with poor glycemic control. Diabetes mellitus is detected by 2.5 times more microorganisms on the skin surface than in healthy individuals, and the bactericidal activity of the skin in patients Diabetes mellitus is lower on average by 20% . This decrease is directly correlated with the severity of diabetes . Infectious-inflammatory diseases primarily develop on the skin of the lower extremities due to angas o- and neuropathies. The cause is usually polymicrobial infections: Staphylococcus aureus, Streptococcus groups A and B, gram-negative aerobic bacteria and many anaerobes. Pyoderma is mainly represented by folliculitis, actima , erysipelas and may be complicated by eczematization . In addition, the development of furunculosis, carbuncles, paronium , soft tissue infections is possible.
On the background of diabetes mellitus, there is an increased frequency of fungal infections, which in the structure of diseases in patients of this category, according to different authors , are 32.5 – 45%.
Under conditions of hyperkalemia, mushrooms actively use sugar for their metabolic processes and multiply vigorously, causing illness. At Diabetes mellitus microcirculation in the vessels of the lower extremities is observed 20 times more often than in individuals without endocrine pathology, which contributes to the development of fungal foot and onychomycosis.
The causative agents of fungal lesions are dermatophytes and Candida. albicans . Moreover, in a normal population, fungal skin lesions caused by C. albicans do not exceed 20%, whereas in somatically burdened patients this figure rises to 80–90%. It should be noted that 80% of the registered candidiasis of the skin is in diabetic patients.
Most common intertrigo (with lesions of the axillary, inguinal areas, interdigital spaces), vulvovaginitis , balanitis , paronychia, glossitis and angular cheilitis. In addition to clinical vaginal yeast infections, patients with diabetes also have an increased incidence of asymptomatic carriage.
Diseases associated with diabetes mellitus and having unclear pathogenesis include lipoid necrobiosis, annular granuloma, diabetic bladder and diabetic dermopathy.
Lipoid necrobiosis (Oppenheim disease – Urbach) is a rare granulomatous chronic disease of a vascular-metabolic nature; it is a localized lipoidosis with deposition of lipids in those parts of the dermis where there is degeneration or necrobiosis of collagen . The first symptoms of dermatosis usually occur in the age group from 20 to 60 years. In childhood, Oppengey-ma-Urbach disease is rare . The incidence of lipoid necrobiosis among patients with diabetes mellitus is 0.1–3%.
The clinical picture of Oppenheim-Urbach disease is very diverse. Various areas of the skin can be involved in the process, but primarily the skin of the front surfaces of the legs. This can probably be explained by the fact that in diabetes, pathological changes initially occur in small vessels of the lower limbs . Lipoid necrobiosis is usually manifested in the form of one or more clearly delimited yellowish-brown plaques. The elements have violet jagged edges that can rise above the skin’s surface or harden. Over time, the elements are aligned and the central yellow or orange area becomes atrophic , often telangiectasias can be seen, which give the affected areas a shine of “glazed porcelain”. Loss of sensation in the area of plaques.
Generalized annular granuloma in 20% of patients is the first symptom of a previously unrecognized type 2 diabetes mellitus . The relationship of the annular granuloma to diabetes mellitus remains a matter of debate, as it may be associated with other diseases . Observed localized, generalized , as well as subcutaneous nodular and perforating forms of annular granuloma associated with diabetes mellitus.
A typical history of an annular granuloma suggests one or more papules growing on the periphery with simultaneous resolution in the center. Outbreaks may retain their natural skin color or be erythematous or purple. The usual sizes of foci are from 1 to 5 cm in diameter. Annular granuloma, as a rule, is asymptomatic; mild pruritus is possible, painful lesions are rarely observed
Diabetic bullosis is subepidermal bullous dermatosis, occurring in patients with diabetes.
For the first time the bubbles as one of the variants of skin lesions observed in diabetes D. Krame r in 1930. A. Cantwell and W. Martz described this condition as diabetic bullosis.
The reason for the appearance of blisters in patients with diabetes is not clear. There are theories about the role of microangiopathy and local metabolic disorders. Diabetic bullosis occurs predominantly in persons with long-term diabetes, and more often in women. The onset of the disease ranges from 17 to 79 years.
On unchanged skin appear blisters ranging in size from a few millimeters to several centimeters (usually on the skin of the lower extremities). There are two types of lesions: intraepidermally located blisters, which disappear without scar formation, and subepidermal blisters, after which atrophied scars remain. Rashes are localized mainly on the feet and shins, but can occur on the hands and forearms. Bubbles spontaneously resolve after 2-5 weeks, relapses are possible.
Atrophic skin changes of the lower extremities, or “spotted lower leg”, were first described and proposed as a marker of diabetes in 1964. Shortly thereafter he coined the term diabetic Binkley “dermopathy” with the aim of correlating the data with those pathological changes ii retinopathy, nephropathy and neuropathy. Diabetic Dermopathy is more common in patients with long-term diabetes and is more common among men. Clinically, it is a small (less than 1 cm) atrophic spots from pink to brown in color and resembling scar tissue, located on the pretibial sites. These elements are asymptomatic and disappear in 1-2 years, leaving behind a small atrophy or hypopigmentation. The emergence of new elements suggests that pigmentation and atrophy are persistent conditions.
Exchange-endocrine disorders are often the trigger for the development of certain dermatoses. There is a certain relationship between the course of these diseases and the presence of endocrinopathy. Severe diabetes mellitus was detected in 19% of patients with lichen planus, in some of them there was a significant change in the glucose tolerance test. Often, oral mucosal lesion in lichen planus combined with diabetes mellitus and arterial hypertension (Potekaeva-Grynszpan syndrome), and rash in the mucosa, usually are erosive-ulcerous character. In a large-scale study to determine the relationship between psoriasis and general health, it was found that women suffering from psoriasis are 63% more likely to develop diabetes, compared with patients who do not have this dermatosis. On the background of diabetes mellitus, psoriasis is more severe, there are such forms as exudative psoriasis, psoriatic polyarthritis, psoriasis large folds.
Thus, changes in the skin may well be associated with systemic disease processes, typical for Diabetes. The basis of the clinical and pathological picture of dermatoses and dermopathies , preceding or developing on the background of diabetes mellitus , are metabolic, vascular, neurological and immune disorders.